What is Crohn's Disease?
Crohn's disease is an inflammatory bowel disease (IBD) that causes chronic inflammation and damage to the gastrointestinal (GI) tract.

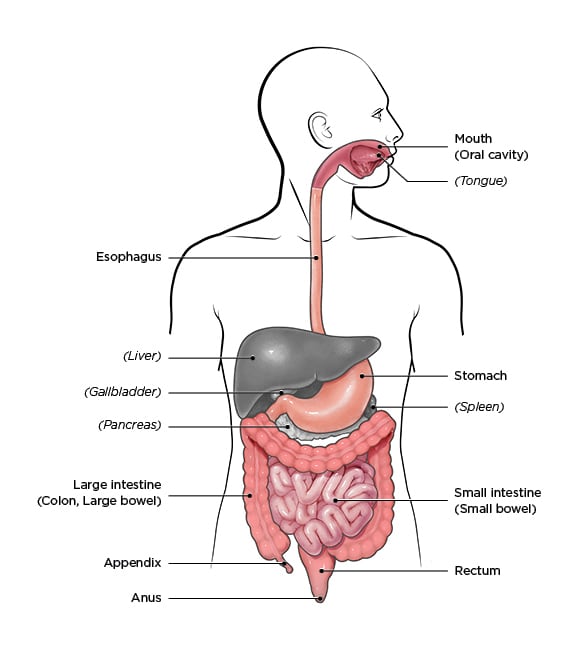
Crohn's disease is an inflammatory bowel disease (IBD) that causes chronic inflammation and damage to the gastrointestinal (GI) tract. Along with ulcerative colitis, it is one of the two main types of IBD. Crohn's can impact any part of the GI tract, from the mouth to the anus, but it most commonly affects the end of the small intestine (the ileum) and the beginning of the colon.
Prevalence and Risk Factors
Around 0.5% of adults in Western countries are estimated to have Crohn's disease. Onset is typically between ages 15 and 35, although Crohn's can develop at any age. Several factors can increase risk, including family history, smoking, ethnicity (higher rates among Ashkenazi Jews and Caucasians), and living in urban and northern climates. The exact cause remains unknown, but research suggests a combination of genetic, immune system, environmental, and microbial factors contribute to developing Crohn's.
Signs and Symptoms
Common symptoms of Crohn's disease include:
- Abdominal pain and cramping
- Persistent diarrhea
- Fatigue and lethargy
- Reduced appetite and weight loss
- Fever and night sweats
- Bloody stools
- Mouth sores
- Perianal complications like fissures or fistulas
Patients experience flares when symptoms worsen, interspersed with periods of remission when symptoms improve. Complications can also arise, such as small intestinal blockages or abscesses.
Diagnosis and Testing
Since there is no single test for Crohn's, physicians combine results from medical history, physical exam, lab tests, endoscopies, and radiology scans to make a diagnosis. Common tests include:
- Blood tests checking for inflammation and anemia
- Fecal calprotectin test to assess GI inflammation
- CT or MRI scans visualizing thickened bowel walls
- Capsule endoscopy to see inside the small intestine
- Colonoscopy with biopsies of abnormal tissue
Treatment Approaches
Treatment focuses on reducing inflammation, managing symptoms, and inducing remission. Options include:
- Medications: anti-inflammatories, immune system suppressors, antibiotics, biologics
- Nutritional therapy: liquid diets, vitamin/mineral supplements
- Surgery: removing severely damaged sections of intestine
- Mental health support: coping with psychological effects
While there is no known cure for Crohn's, proper treatment and lifestyle adjustments can help patients achieve long-term remission and improved quality of life.

Useful links for Crohn's sufferers.